Recognizing early liver problems allows you to intervene before irreversible damage occurs, safeguarding your overall vitality as you age. Your liver works tirelessly to filter toxins, process nutrients, and produce essential proteins, making the detection of subtle liver warning signs critical. Because the liver rarely shows obvious symptoms until diseases advance, learning to spot signs of liver damage can be truly lifesaving. For adults over 60, age-related changes and accumulated exposure to medications increase vulnerability to hepatic stress. Paying attention to fatigue, mild skin changes, or digestive shifts empowers you to seek timely medical care. You possess the ability to improve liver health simply by tuning into the quiet signals your body sends every day.
Understanding the Basics of Liver Function
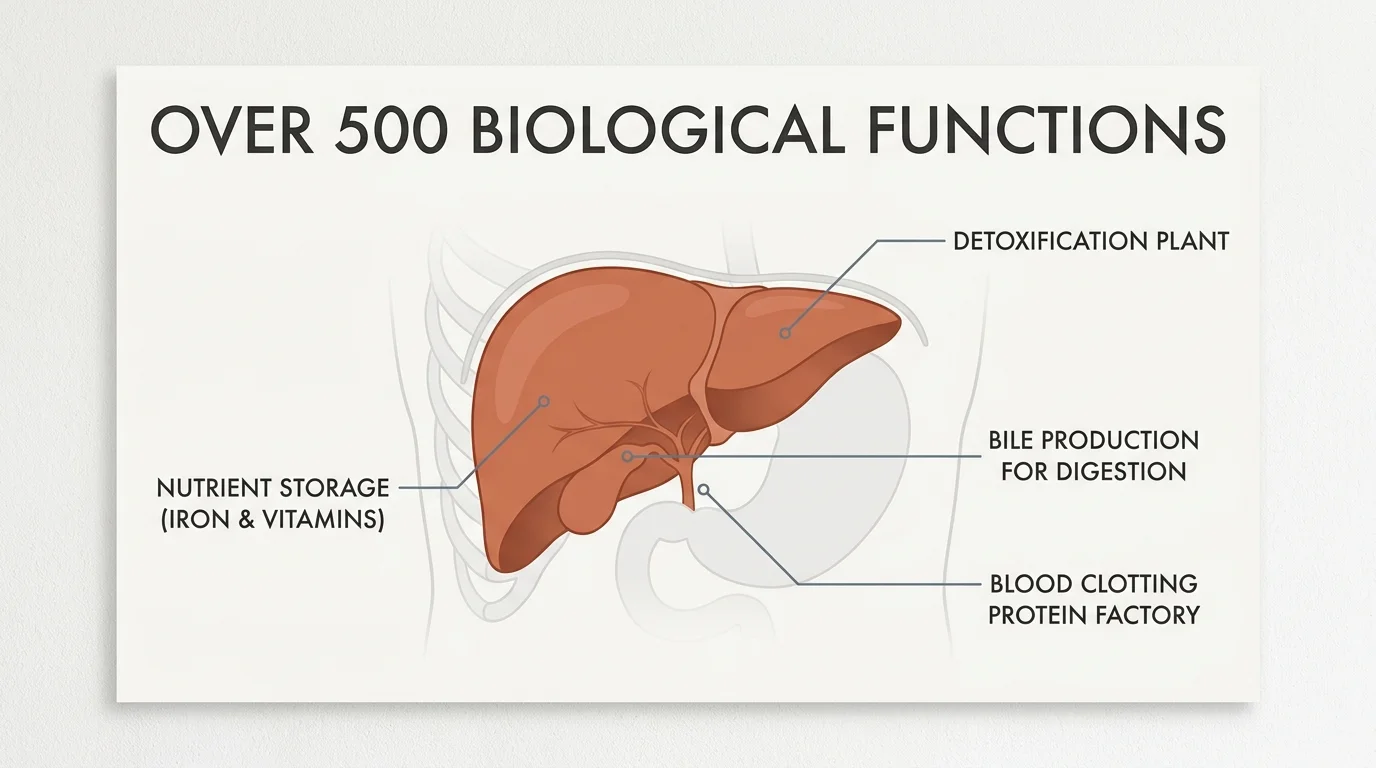
You probably rarely think about your liver until a routine blood test reveals an abnormality or you experience unexplainable discomfort. Yet, this remarkable organ serves as your body’s primary filtration system and metabolic powerhouse. Weighing approximately three pounds and sitting quietly in the upper right side of your abdomen, your liver performs over five hundred distinct biological functions essential for your survival. It acts as a highly sophisticated chemical processing plant. Every single thing you consume—from daily meals and occasional alcoholic beverages to prescription medications and environmental toxins—must eventually pass through the liver for detoxification and metabolism.
Beyond simply filtering out harmful substances, your liver produces bile to help digest fats, stores vital nutrients like iron and vitamins, and manufactures the specialized proteins required for your blood to clot properly. When your liver operates at peak efficiency, your energy levels remain consistently stable, your digestion works smoothly without interruption, and your immune system readily fights off seasonal infections.
However, this stoic organ rarely complains when it first encounters physiological stress. Unlike a strained muscle or a skin burn that sends immediate, sharp pain signals to your central nervous system, early liver problems develop in complete silence. The liver possesses an incredible, unique capacity to regenerate damaged tissue; it routinely compensates for minor injuries by replacing compromised cells with healthy, functioning ones. While this regenerative ability is a biological marvel, it also presents a significant danger to your long-term health. Because the liver works so incredibly hard to mask its struggles and maintain normal bodily functions, significant scarring—known medically as fibrosis—can develop long before you ever notice the classic liver health symptoms. Understanding the foundational role this crucial organ plays in your overall physiology highlights exactly why you must remain vigilant and proactive.
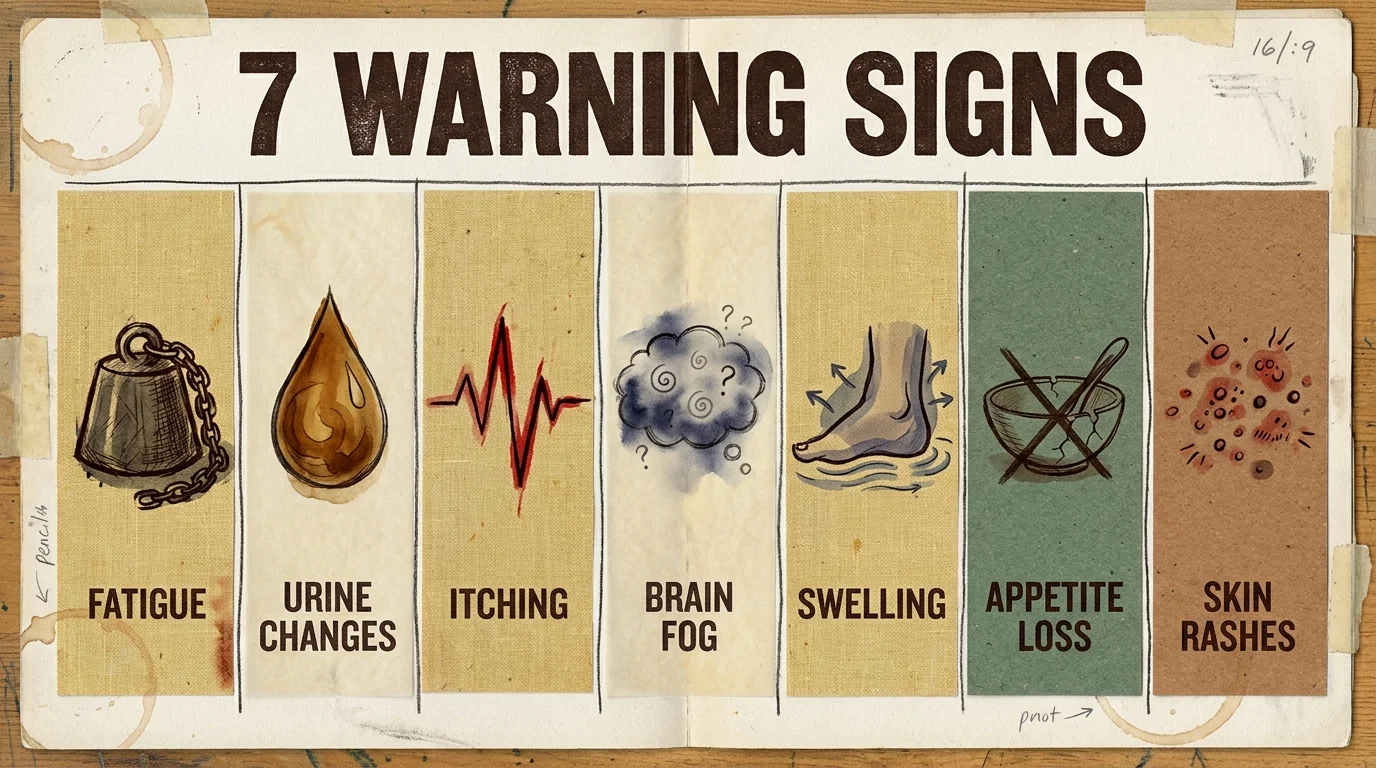
The 7 Early Warning Signs Your Liver Is Struggling
Catching liver dysfunction in its infancy requires paying close attention to systemic shifts that you might otherwise write off as normal signs of aging. The body provides several subtle clues when hepatic stress begins to outpace cellular regeneration. By learning to identify these seven warning signs, you can catch early liver problems before they evolve into irreversible conditions.

1. Unexplained Fatigue and Profound Weakness
While everyone experiences occasional tiredness after a busy day, the fatigue associated with a struggling liver feels entirely different. When liver function declines, your body loses its ability to efficiently store and release glucose. Without a reliable, steady supply of energy circulating through your bloodstream, you will feel thoroughly exhausted even after a full night of restful sleep. Furthermore, a compromised liver struggles to clear metabolic waste products from your system. This buildup of systemic toxins triggers an inflammatory immune response, prompting your body to release cytokines. Cytokines are chemical messengers that induce a profound, unshakeable sense of lethargy. If you suddenly find yourself needing long daytime naps just to function, your liver might be working overtime to manage an overload of toxins.
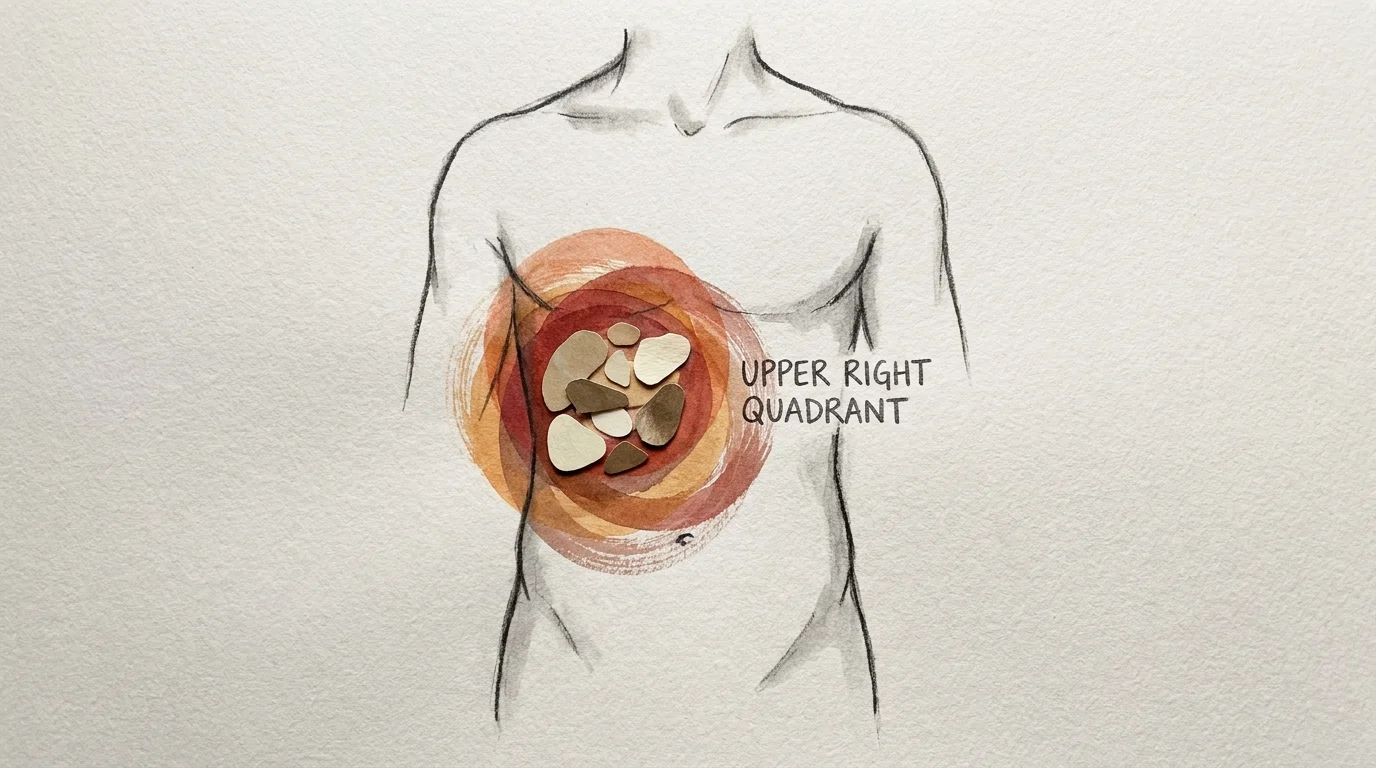
2. Right-Sided Abdominal Discomfort or Fullness
Interestingly, the liver itself contains no actual pain receptors, meaning the organ cannot directly feel pain. However, it is surrounded by a thin, nerve-dense protective layer known as Glisson’s capsule. When your liver becomes inflamed or swollen due to fat accumulation, viral infections, or toxicity, the organ physically expands and stretches this sensitive capsule. This stretching results in a dull, persistent ache or a sensation of heavy fullness in the upper right quadrant of your abdomen, just beneath your lower rib cage. You might notice this discomfort worsening after eating a particularly heavy, high-fat meal, as the liver and gallbladder strain to produce and release enough bile for digestion.
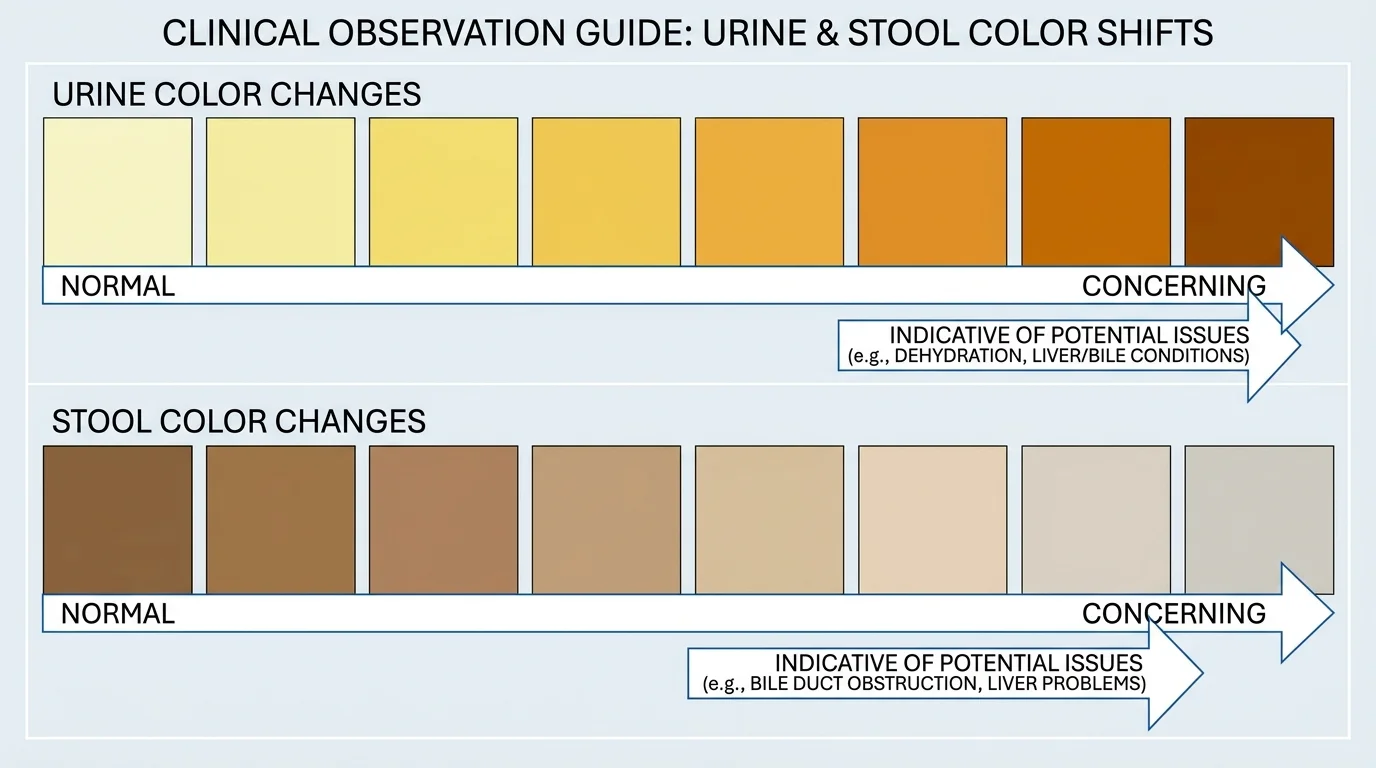
3. Noticeable Changes in Urine and Stool Color
Your bathroom habits offer a highly accurate window into your internal metabolic health. The liver continuously processes a yellowish-orange pigment called bilirubin, which is created during the normal, daily breakdown of old red blood cells. A healthy liver effectively extracts this bilirubin from your blood, mixes it into bile, and excretes it through your digestive tract, giving healthy stool its typical brown color. If your liver becomes sluggish or damaged, it cannot process bilirubin efficiently. The excess pigment spills over into your kidneys, causing your urine to turn remarkably dark—resembling the color of amber or dark tea—even when you are fully hydrated. Simultaneously, a lack of bilirubin reaching your intestines will cause your stool to appear unusually pale, clay-colored, or putty-like.

4. Persistent, Unexplained Skin Itchiness
Pruritus—the medical term for severe, unrelenting itchy skin—frequently serves as an early indicator of a liver under distress. Unlike allergic reactions or contact dermatitis, the itchiness associated with liver dysfunction typically occurs without any visible rash, hives, or skin flaking. Medical researchers believe this phenomenon occurs when the liver fails to properly filter bile salts. These acidic salts subsequently escape into the bloodstream and accumulate directly beneath the surface layers of your skin. The itching often becomes far more intense during the late evening and nighttime hours, particularly affecting the palms of your hands and the soles of your feet. Because this symptom seems entirely unrelated to internal organs, many seniors spend months trying topical lotions and dermatological treatments before uncovering the true hepatic root cause.

5. Mild Fluid Retention in the Legs and Abdomen
A healthy liver constantly produces albumin, a crucial protein that acts like a biological sponge to keep fluid safely contained within your blood vessels. When liver function drops, albumin production plummets right alongside it. Without enough albumin circulating in your blood, fluid begins to leak out into the surrounding bodily tissues. Initially, you might notice this as mild swelling—known as edema—around your ankles, feet, and lower legs at the end of the day. As the pressure within the blood vessels supplying the liver increases—a condition called portal hypertension—fluid may also begin to pool inside the abdominal cavity. This specific type of abdominal swelling, called ascites, can make your clothes feel suddenly tight and cause uncomfortable bloating.
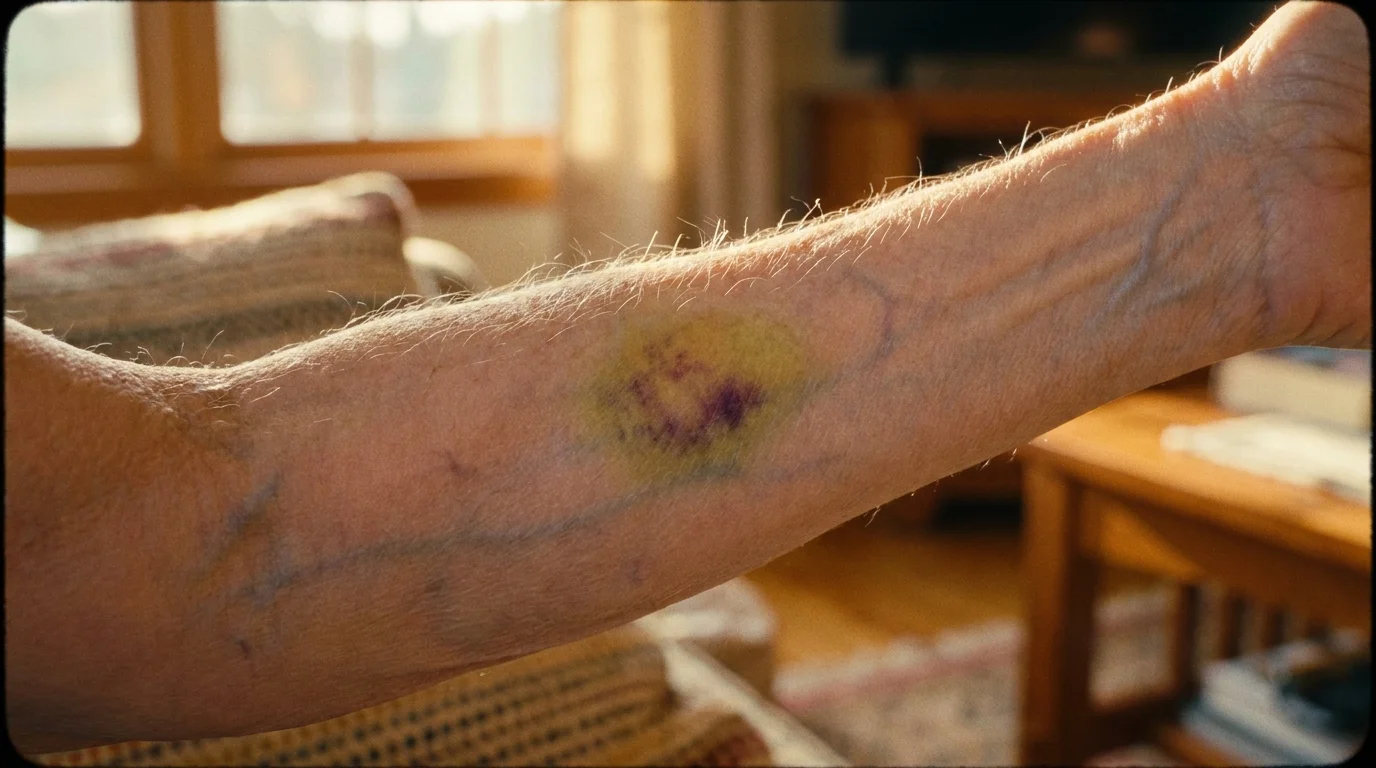
6. Easy Bruising and Prolonged Bleeding
Your liver acts as the primary manufacturing center for blood-clotting factors, which are specialized proteins necessary to stop bleeding after an injury. As liver tissue sustains damage and normal cellular function declines, the production of these critical clotting factors slows down significantly. You might begin to notice large, dark bruises appearing on your arms and legs from incredibly minor bumps that you hardly even felt. Additionally, you may experience frequent nosebleeds, notice bleeding from your gums when you brush your teeth, or find that small paper cuts take an unusually long time to stop bleeding. Recognizing this sign of liver damage is crucial, as compromised clotting abilities present a severe risk during accidental falls or emergency surgeries.

7. Mild Cognitive Confusion and Brain Fog
Perhaps one of the most alarming early warning signs of a struggling liver involves sudden shifts in your cognitive clarity. During the normal digestion of protein, your body produces ammonia as a toxic byproduct. A healthy liver quickly intercepts this ammonia and converts it into urea, which is safely excreted in your urine. A struggling liver, however, allows ammonia levels to rise and circulate freely throughout the body. When this toxic ammonia crosses the blood-brain barrier, it disrupts normal neurotransmitter function. In its early stages, this condition—known as hepatic encephalopathy—manifests as mild brain fog, difficulty concentrating on daily tasks, unusual forgetfulness, or changes in your normal sleep-wake cycle. Families often mistake these early cognitive shifts for normal age-related memory loss, completely missing the underlying liver crisis.

Key Considerations for Aging Adults
Addressing liver health symptoms requires a deep understanding of how aging physically alters your internal organs. As you transition from middle age into your senior years, your liver naturally undergoes several significant physiological changes. For instance, overall liver volume decreases by roughly twenty to forty percent as you age. Furthermore, the volume of blood flowing through the liver declines significantly, meaning the organ receives less oxygen and fewer nutrients to support rapid cellular regeneration.
This reduction in blood flow carries massive implications for how your body processes chemicals. Older adults often face the challenge of polypharmacy—the simultaneous, daily use of multiple prescription medications, over-the-counter pain relievers, and various dietary supplements. Because the aging liver processes these substances at a much slower rate, active drug compounds remain in your bloodstream far longer than they would in a younger body. This prolonged exposure dramatically increases the risk of accidental drug-induced liver injury. A dose of acetaminophen or a statin medication that was perfectly safe in your forties might overwhelm your reduced liver capacity in your seventies.
Additionally, the compounding effects of an aging metabolism make seniors particularly vulnerable to metabolic dysfunction-associated steatotic liver disease, a condition where excess fat accumulates directly inside liver cells. Changes in body composition, specifically the tendency to store more visceral fat around the abdomen after age sixty, place constant inflammatory stress on hepatic tissues. Therefore, older adults must approach liver health with a heightened level of awareness, recognizing that their bodies possess less metabolic leniency than they did in previous decades.
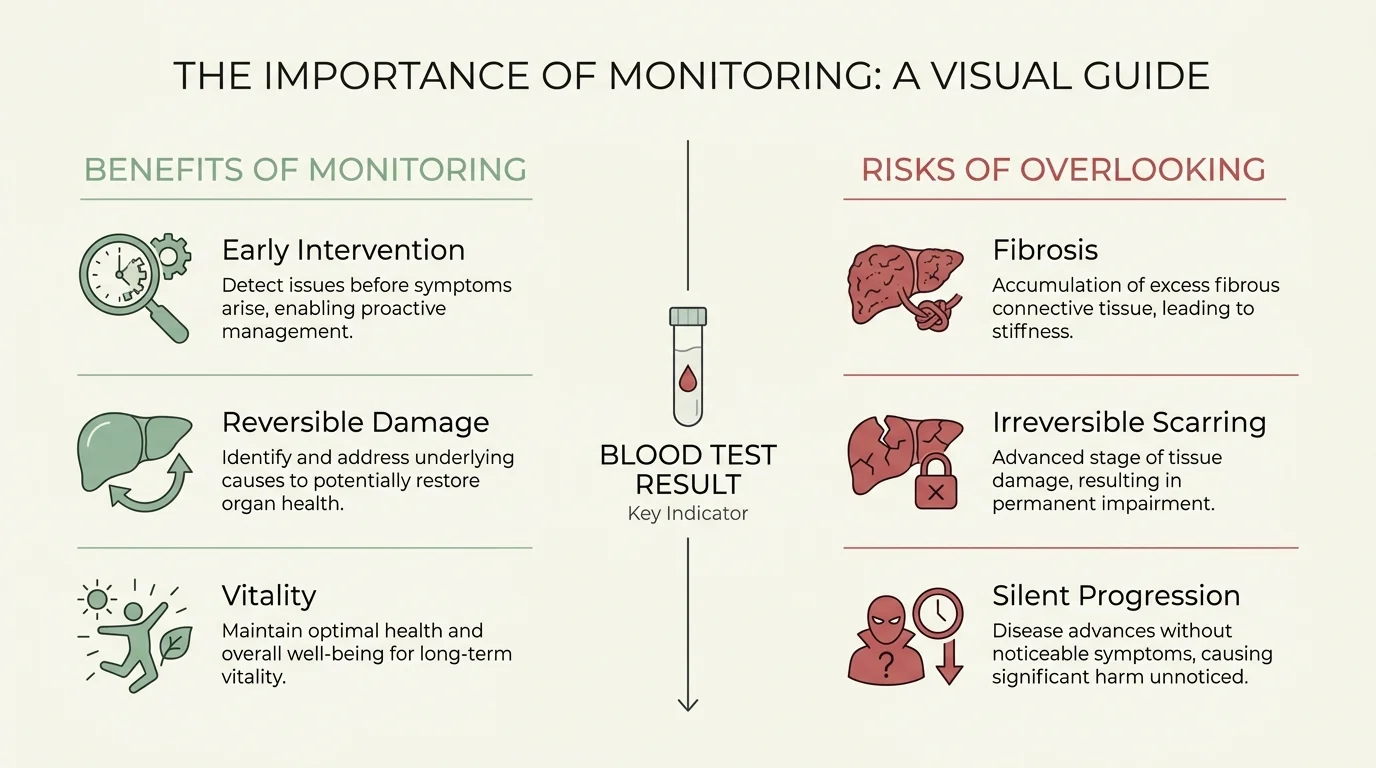
Benefits and Potential Risks of Monitoring Your Liver
The primary benefit of monitoring your body for early liver problems lies in the incredible reversibility of early-stage liver disease. When you catch fatty liver disease, mild inflammation, or early toxicity before scar tissue solidifies, you can often restore your liver to perfect health through targeted lifestyle modifications. Recognizing these early signs empowers you to make dietary shifts, adjust harmful medications, and eliminate toxins, ultimately protecting yourself from the devastating complications of late-stage cirrhosis, liver failure, or hepatocellular carcinoma. Improved liver function translates directly into more abundant daily energy, clearer cognitive focus, and a significantly stronger immune response.
Conversely, there are potential psychological risks to hyper-fixating on subtle physical changes. Because many early warning signs your liver is struggling—such as generalized fatigue or mild brain fog—overlap heavily with other common ailments, you risk generating unnecessary medical anxiety. Assuming that every bout of tiredness indicates organ failure can lead to severe stress, which ironically harms your overall health. Furthermore, there is the risk of falling into the trap of self-diagnosis. Attempting to treat suspected liver issues with unverified, over-the-counter “liver detox” supplements can actually cause acute toxic damage. The goal is vigilant awareness, not panic; recognizing symptoms should solely serve as the catalyst for scheduling a professional medical evaluation.
What the Experts Say About Hepatic Health
Leading medical organizations emphasize that liver disease is no longer solely associated with heavy alcohol consumption. Experts from the National Institutes of Health constantly warn the public about the hidden epidemic of fatty liver disease driven by metabolic syndrome, type 2 diabetes, and high cholesterol. They stress that the modern Western diet, which is heavily reliant on ultra-processed foods and high-fructose corn syrup, places unprecedented demands on the human liver.
Similarly, researchers at the Mayo Clinic advocate for routine metabolic screenings, particularly for older adults carrying excess abdominal weight. They highlight that early intervention through sustained weight management and physical activity remains the most highly effective, scientifically proven treatment for reversing early fat accumulation in the liver. There is no magic pill for hepatic health; instead, the medical consensus points entirely toward systemic metabolic care.
Public health guidelines from the Centers for Disease Control and Prevention also heavily underscore the importance of viral hepatitis screenings for older populations. The organization recommends that all adults get screened for Hepatitis C at least once in their lifetime, as this stealthy virus can silently damage the liver over several decades without producing a single recognizable symptom until severe cirrhosis has already taken hold.
Practical Steps to Improve Liver Health Today
You can begin protecting your hepatic health immediately by executing a comprehensive medication audit. Schedule an appointment with your primary care physician or a licensed pharmacist to review every single pill you consume daily. This review must include all prescription drugs, over-the-counter pain relievers, herbal supplements, and daily vitamins. Identifying redundant medications or supplements that tax the liver unnecessarily is often the fastest way to relieve metabolic stress.
Transitioning your daily nutritional habits toward a Mediterranean-style diet offers profound, scientifically backed benefits for liver function. Prioritize eating robust leafy greens, cruciferous vegetables like broccoli and Brussels sprouts, and lean proteins like wild-caught fish. These specific foods contain powerful antioxidants and sulfur compounds that actively assist the liver in its detoxification processes. Simultaneously, you must ruthlessly eliminate highly processed food items and heavily sweetened beverages, as liquid fructose causes immediate fat accumulation within hepatic cells.
Staying adequately hydrated provides the physical medium your liver needs to flush toxins effectively from your body. Aim to drink clean, filtered water consistently throughout the day. Interestingly, drinking black coffee in moderation provides excellent hepatic support; numerous clinical studies demonstrate that the specific antioxidants found in coffee beans help prevent the buildup of liver fat and reduce collagen deposition, effectively slowing down the progression of fibrosis.
Finally, completely reevaluate your alcohol consumption. Because an aging liver processes alcohol much slower, toxins linger in your bloodstream and inflict significantly more cellular damage. Eliminating alcohol entirely, or reducing your intake to strictly special occasions, offers your liver the biological breathing room it desperately needs to regenerate damaged tissue.
Frequently Asked Questions
Can the liver truly repair itself after sustaining damage?
Yes, the liver possesses a remarkable, unique capacity to regenerate lost or damaged tissue. If you intervene during the early stages of fat accumulation or mild inflammation, the organ can often heal completely. However, once continuous damage causes severe, hardened scar tissue—known as cirrhosis—the damage becomes permanent and irreversible. Early detection remains the ultimate key to healing.
Are elevated liver enzymes on a blood test always a cause for immediate panic?
Elevated liver enzymes, such as ALT and AST, indicate that liver cells are currently inflamed or dying off, but they are not a reason to panic. A temporary spike can result from a recent viral infection, a strenuous physical workout, or a newly prescribed medication. Your doctor will use these elevated markers as a starting point to investigate further, often ordering an ultrasound or a repeat blood test to determine the exact underlying cause.
How does routine alcohol consumption affect the liver as we age?
As you age, your body contains less water volume and your liver metabolic enzymes decrease in efficiency. Consequently, your blood alcohol concentration rises much higher and faster than it did in your youth, even if you drink the exact same amount. This prolonged exposure accelerates hepatic cellular death and significantly increases your risk of developing alcoholic liver disease later in life.
What specific role does body weight play in liver function?
Carrying excess weight, specifically visceral fat that tightly wraps around your abdominal organs, directly contributes to metabolic dysfunction. This fat is biologically active; it releases inflammatory chemicals directly into the portal vein that feeds the liver. Losing just five to ten percent of your total body weight can dramatically reduce liver fat, ease systemic inflammation, and rapidly improve liver function.
Can seemingly harmless over-the-counter pain relievers cause liver stress?
Absolutely; over-the-counter medications like acetaminophen are metabolized directly by the liver. While generally safe when taken exactly as directed, accidentally exceeding the maximum daily dosage can cause acute, severe liver failure within a matter of days. Seniors must carefully read all medication labels, as acetaminophen is frequently hidden inside multi-symptom cold and flu remedies, making accidental overdoses dangerously easy.
Closing Thoughts on Hepatic Wellness
Protecting your liver requires a proactive mindset and a willingness to listen closely to your body. By understanding the foundational role this organ plays in your overall vitality, you can better appreciate the critical importance of early detection. Unexplained fatigue, right-sided abdominal fullness, dark urine, itchy skin, fluid retention, easy bruising, and cognitive brain fog all serve as the early warning signs your liver is struggling to keep up with metabolic demands. As an older adult, evaluating your daily medications, adopting a nutrient-dense diet, and communicating openly with your healthcare provider will ensure your liver continues to support you for decades to come. Taking action today allows you to preserve your physical independence and secure a much healthier, more vibrant tomorrow.
This article is intended for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with a qualified healthcare provider regarding any health concerns or before making any decisions related to your health or treatment.